Amblyopia refers to reduced vision in one or both eyes caused by visual deprivation. Normal vision is “imprinted” in the brain in early childhood. If this process is interrupted, amblyopia will occur.
WHAT IS AMBLYOPIA?
Amblyopia refers to reduced vision in one or both eyes caused by visual deprivation in childhood. That is, even with proper eyeglasses, an eye with amblyopia does not see well! It is often reversible with the appropriate treatment. The term “lazy eye” is often used to describe amblyopia.
Amblyopia results from actual atrophy of the visual pathways in the brain that allow an individual eye to “see.” That is, because of improper stimulation of the involved eye, the portion of the brain serving that eye does not develop properly. Amblyopia affects approximately 2% of all children. There is often a family history of this disorder.
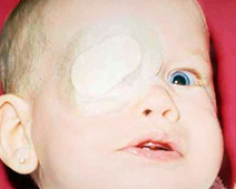
Eye patch worn over this child’s right eye to reverse amblyopia in the left eye.
WHAT CAUSES AMBLYOPIA?
The causes of amblyopia are varied and include:
- Strabismus (crossed-eyes). This refers to any misalignment of the eyes. When the eyes are not aligned, the child’s brain will often select one eye to view the world while the other will be “shut off” or “suppressed”. The eye that is habitually deviated or crossed is at risk for developing amblyopia.
- Anisometropia. This refers to an unequal eyeglass prescription between the eyes. If eyeglasses are not worn, then the eye that receives the more blurred images (the eye with the higher eyeglass prescription) is at risk for developing amblyopia.
- Visual occlusion. Any ocular disease that blocks the visual images from reaching the back surface of the eye (retina) can cause amblyopia. Examples include congenital cataracts, corneal opacities or droopy eyelids (ptosis). Even if the underlying disease is corrected with the appropriate surgery, a significant amblyopia may persist.
The extent of visual loss due to amblyopia ranges from mild to severe.
What are the Signs of Amblyopia?
Unless an obvious abnormality is present (e.g. crossing of the eyes, a droopy eyelid or a dense cataract), amblyopia may have no obvious signs. When only one eye is affected, a young child will not usually complain of blurred vision or exhibit any unusual visual behavior.
Fortunately, young children undergo vision screening periodically at their pediatrician’s office and at school to detect amblyopia.
MAKING THE DIAGNOSIS
The pediatric ophthalmologist performs all of the necessary tests to confirm that your child has amblyopia.
Vision testing is accomplished with the appropriate methods for your child’s age.
An examination with eye drops that dilate the pupils is generally performed. This permits an evaluation of the internal ocular structures and allows a determination as to whether or not there is a need for eyeglasses.
Treatment
The key to successful treatment of amblyopia, is early detection. See Vision Screening for more information.
If the amblyopia is caused by a strabismus, patching therapy is generally recommended.
If an anisometropic amblyopia is present, the proper eyeglasses are prescribed, possibly in conjunction with patching therapy.
If there is a cataract or other ocular anomaly present, the appropriate surgery may be recommended.
Eye Patch Therapy
For achieving the best results in amblyopia therapy, total visual deprivation of the stronger eye is often recommended. For this reason, eye patches that adhere to the skin around the eye are most effective. Strap-on “pirate’s patches” and patches worn over glasses are less effective and only occasionally recommended.
Particularly if a child is resistant to patching therapy, “atropine” eyedrops may be helpful in certain conditions. Atropine is instilled onto the dominant eye creating a temporary blurring effect which may allow the child to use the other eye with amblyopia – thus “patching without a patch.”
The pediatric ophthalmologist will prescribe the appropriate number of hours that the patch should be worn each day. While undergoing patching or atropine eyedrop therapy, it is critical that your child return for a vision check at the recommended time intervals! This is to safeguard against the development of amblyopia in the eye being patched.
Generally, the younger the child, the quicker the desired results are obtained with amblyopia therapy. After about age 11 years, the benefit of patching or atropine therapy is questionable.
What if My Child Refuses to Wear the Patch?
It is not uncommon that children with amblyopia will refuse to wear the patch and remove it when left unsupervised.
Patching should commence during a time when you can devote all of your attention to your child (e.g. weekend). Typically, the first few days are the most difficult. Keep your child occupied with games or television when wearing the patch. If your child removes the patch, promptly replace it. Let your child know that you are the boss! Bribery may sometimes be necessary.
In some younger children, the use of socks over the hands taped to the wrists may be required. Sometimes, elbow splints are needed to prevent a child from removing the patch.
FREQUENTLY ASKED QUESTIONS
Can surgery correct amblyopia? No.
If not treated, can my child outgrow amblyopia? No.
If my child has amblyopia, should his/her siblings be evaluated by an ophthalmologist? It is reasonable that all siblings of children diagnosed with anisometropic amblyopia have a baseline examination by an ophthalmologist at age 3–4 years.
Pediatric Ophthalmic Consultants
40 West 72nd Street, New York, 10023 | 212-981-9800
The content of this Web site is for informational purposes only. If you suspect that you or your child has any ocular problem,
please consult your pediatrician, family practitioner, or ophthalmologist to decide if a referral to a pediatric ophthalmologist is required.