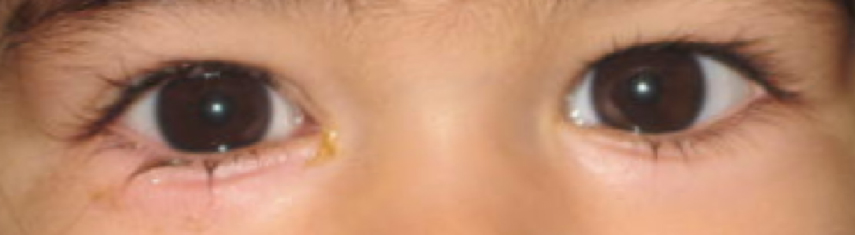
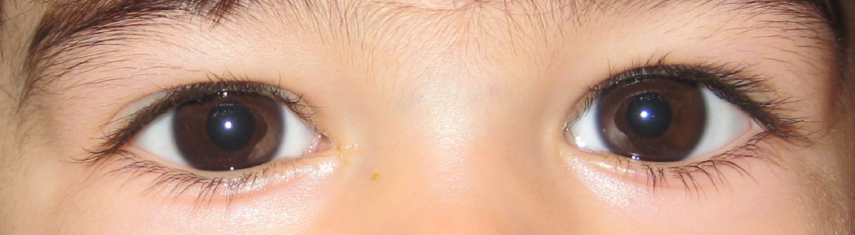
This refers to a blockage of the drain that empties tears from the eyes. Usually present at birth, a child with a tear duct obstruction will have excessive tears and at times discharge and crusting on the eye surface.
WHAT IS A TEAR DUCT OBSTRUCTION?
The tears are constantly manufactured by glands within the eyelids. After lubricating the eye, the tears normally drain into two small holes (“puncta”) located on the inner corner of the upper and lower eyelids. From there, the tears drain into the back of the nose via the tear duct (a.k.a. nasolacrimal duct). This is why we tend to have a runny nose when we cry! Infants with a nasolacrimal duct obstruction typically have a blockage at the most distant end of the duct immediately before it empties into the nose.
Approximately six percent of all infants are born with a nasolacrimal duct obstruction (tear duct blockage) affecting one or both eyes. Fortunately, at least 90% of these obstructions will clear without treatment within the first year of life.
WHAT ARE THE SIGNS OF A TEAR DUCT OBSTRUCTION?
As the tears have nowhere to drain, they will well up on the surface of the eye and often overflow onto the eyelashes, lids and cheek. Normally there are bacteria in the tears which also have nowhere to drain when a blockage is present. These bacteria tend to grow within the tear duct and cause a pus-like discharge from the inner corner of the eye and on the lashes — frequently observed when the child awakens.
MAKING THE DIAGNOSIS
The pediatric ophthalmologist will perform all of the necessary tests to confirm that your child has a tear duct obstruction. Other rarer causes of tearing in children will be ruled-out.
Treatment
As the majority of tear duct obstructions will resolve without any intervention by age 12 -18 months, conservative measures are usually recommended. The typical treatment protocol includes:
- Tear duct massage (as demonstrated by the doctor) three times each day if any signs of a tear duct obstruction are evident.
- Antibiotic eye drops three times daily as needed after the massage. These eye drops should be used only when a yellow or green pus-like discharge is present throughout the day. The eye drops should be discontinued if only a white mucus-like discharge or no discharge is present.
PROBING
A probing of the nasolacrimal duct is a surgical procedure performed to relieve the obstruction for any of the following reasons:
- If the tearing in combination with a frequent pus discharge persists after the first birthday.
- If the pus discharge persists despite use of the antibiotic eye drops and massage.
- If a more serious infection of the tear duct (“dacryocystitis”) or infection of the skin over the tear duct occurs as a result of the obstruction.
- If the tearing persists even in the absence of pus discharge at age 18+ months.
This delicate procedure is safely performed when your child is motionless. This is best achieved with a brief “mask” anesthesia at a hospital outpatient surgical facility.
During the probing, a small smooth wire probe is passed through the tear duct and into the nose. The surgeon confirms an open tear drainage system at the end of this procedure. Often a silicone stent is placed in the tear duct during this procedure and left in place for 6 months to assure that the blocked duct does not close again after the probing. The silicone stents are easily removed in the surgeon’s office without any need for anesthesia.
There are no incisions or scarring from this operation. There is no significant post-operative discomfort.
The vast majority of tear duct probing procedures are successful and do not require additional surgery.
Pediatric Ophthalmic Consultants
40 West 72nd Street, New York, 10023 | 212-981-9800
The content of this Web site is for informational purposes only. If you suspect that you or your child has any ocular problem,
please consult your pediatrician, family practitioner, or ophthalmologist to decide if a referral to a pediatric ophthalmologist is required.